FAQ'S Total hip replacement
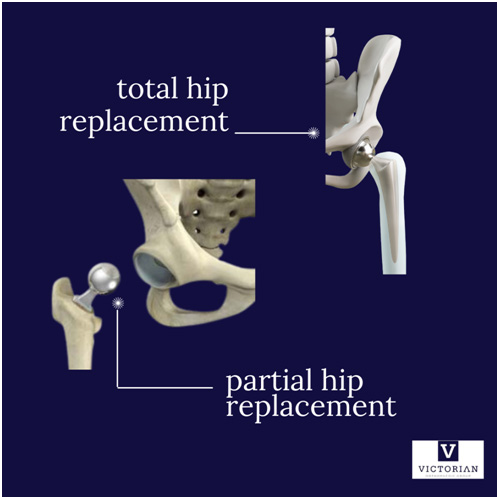
There are primarily two types of hip replacement surgeries: Total Hip Replacement (THR) and Partial Hip Replacement (Hemiarthroplasty).
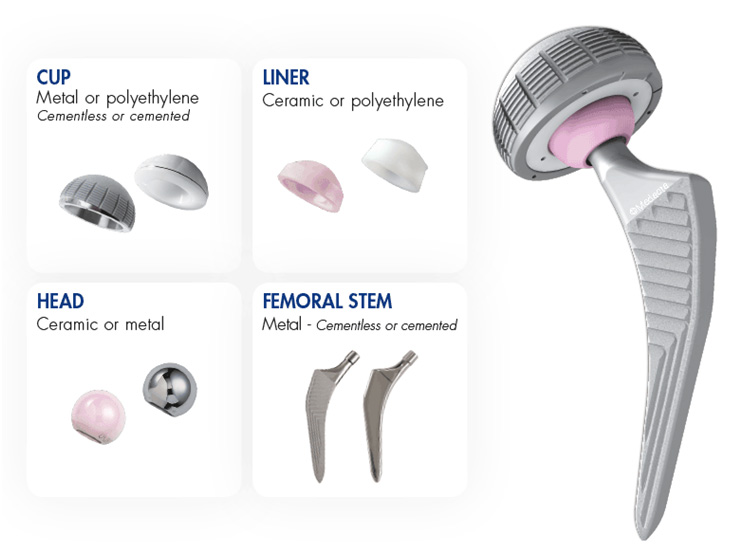
Total Hip Replacement (THR):In a Total Hip Replacement, both the ball (femoral head) and the socket (acetabulum) of the hip joint are replaced with artificial components. These components can be made from materials such as metal, plastic, or ceramic. THR is highly effective for treating advanced arthritis and severe hip joint damage, providing significant pain relief and improved joint function.
Partial Hip Replacement (HemiarthroplastyA Partial Hip Replacement involves replacing only the femoral head (the ball portion of the hip joint) with a prosthetic component, leaving the natural socket intact. This procedure is typically performed when the hip socket remains healthy, such as in cases of femoral neck fractures, particularly in elderly patients.
Comparison of Anterior and Posterior Approach Total Hip Replacement Surgery
| ANTERIOR APPROACH | POSTERIOR APPROACH |
| Access Point: Front of the hip | Access Point: Back of the hip |
Muscle Sparing: Does not cut major muscles | Muscle Preservation: Involves cutting some muscles and tendons |
| Recovery Time: Typically, quicker, with less post-operative pain | Recovery Time: Usually longer, with more post-operative restrictions |
| Visibility and Access: Less visibility, but avoids muscle cutting | Visibility and Access: Excellent visibility, ideal for complex cases |
| Post-Operative Mobility: Patients can often bend their hip and bear weight immediately | Post-Operative Mobility: Patients need to avoid certain movements to prevent dislocation |
| Post-Operative Precautions: | Post-Operative Precautions: |
| – Limit hip extension for six weeks following the surgery | – Avoid combined bending and turning of the hip – Avoid Twisting Movements: Keep your hips aligned and avoid twisting at the waist to maintain the stability of your new hip joint. – Limit Bending: When bending forward, do not go beyond 90 degrees at the hip. This precaution helps prevent dislocation. – No Crossing Legs: Avoid crossing your legs or ankles, as this can put undue pressure on your hip and disrupt the healing process. – Sleep with a pillow between legs for 6 weeks |
| Suitability: Often preferred for quicker recovery and fewer restrictions | Suitability: Suitable for complex cases requiring better visibility |
| Technological Integration: Often involves advanced imaging and planning technologies | Technological Integration: Standard practice with established techniques |
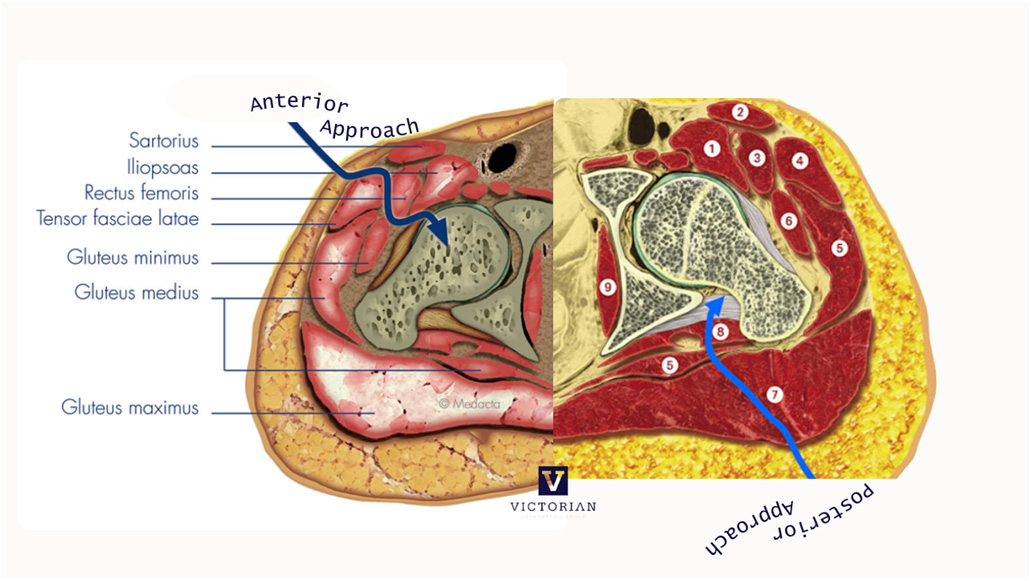
Dr Scott Tulloch utilises advanced imaging and planning technologies to determine the most suitable approach for each patient, ensuring optimal outcomes and a personalised recovery plan. This comparison will help you understand the differences between the anterior and posterior approaches to hip replacement surgery, enabling you to make an informed decision about the procedure that best suits your needs.
Understanding the anaesthetic process is crucial for those undergoing hip replacement surgery, as it ensures a comfortable and safe surgical experience.
Objectives of Anaesthesia:
- Anaesthesia: Achieving a state of controlled unconsciousness for the duration of the surgery to ensure you are unaware and unresponsive.
- Analgesia: Providing effective pain relief during surgery to mitigate the stress response to the surgical procedure.
- Prevention Measures: Implementing strategies to prevent deep vein thrombosis (DVT) and avoid pressure sores or nerve damage due to positioning during the operation.
- Post-Operative Analgesia: Ensuring ongoing pain relief following the surgery to support your recovery.
Anaesthetic Techniques for Hip Replacement Surgery:
General Anaesthesia:
- Involves being completely unconscious and unaware of the surgery.
- To aid post-operative pain relief, additional local or regional anaesthesia may be administered while you’re under general anaesthesia.
Regional Anaesthesia:
- Often accompanied by sedation, regional anaesthesia for hip surgery typically involves a spinal or, less commonly, an epidural anaesthetic.
- This method numbs the lower limbs by blocking nerves in the lower back, with effects lasting 3-4 hours to cover the surgery duration.
Many patients expect general anaesthesia for their operation but are surprised to learn that regional anaesthesia, coupled with sedation, is frequently preferred for joint replacement surgeries due to its benefits in pain management and recovery.
Sedation and Patient Experience:
Sedation:
- Sedation, while optional, is often recommended due to the operational noise.
- The level of sedation is tailored to each patient’s comfort, ensuring a peaceful experience.
- Continuous monitoring by the anaesthetist allows for adjustments in sedation levels as needed.
- Most patients remember little of the procedure, often mistaking their sedation for general anaesthesia.
Choosing the Best Anaesthetic Approach:
The choice of anaesthesia is influenced by your medical history, previous anaesthetic experiences, and personal preferences. Dr Tulloch and the anaesthetic team are open to discussing the best anaesthetic approach for you, ensuring your comfort and safety are prioritised.
General Anaesthesia vs Regional Anaesthesia:
Aspect | General Anaesthesia | Regional Anaesthesia |
Consciousness | Complete unconsciousness | Conscious with numb lower limbs; often paired with sedation |
Pain Management | Additional local/regional anaesthesia for post-operative pain relief | Effective during surgery with extended pain relief post-operatively |
Recovery | Longer recovery time and higher potential for nausea and grogginess | Faster recovery, less nausea, and better immediate post-op pain control |
Sedation Level | Not required as patient is fully unconscious | Tailored sedation for comfort during surgery noise and overall experience |
Total hip replacement surgery typically takes between 1 to 2 hours to complete. The exact duration can vary depending on several factors, including the complexity of the surgery, the specific surgical approach used, and the individual patient’s anatomy and health condition.

Surgical Approach: The chosen surgical technique can influence the duration. For example, the direct anterior approach, which is minimally invasive, might take slightly longer due to the careful navigation around muscles and tissues. Conversely, more traditional approaches like the posterior method may be quicker but involve different considerations for muscle and tissue management.
Patient Factors: The overall health of the patient, including the presence of pre-existing conditions and the extent of damage to the hip joint, can also impact the time required for surgery. More complex cases, such as those involving significant joint deformities or previous hip surgeries, might extend the surgical time.
Pre-Operative Preparation: Before the surgery begins, there is also time allocated for anaesthesia, positioning the patient, and preparing the surgical site. This preparation typically adds some time to the overall procedure.
Post-Operative Care: Following the surgery, patients are moved to the recovery area, where they are closely monitored as the anaesthesia wears off. This phase is not included in the surgical time but is an important part of the overall procedure.
Dr Scott Tulloch is committed to providing detailed information during your consultation, including what you can expect in terms of the duration of your surgery and the specific factors that might influence this for your individual case. The focus is on ensuring a safe and successful procedure, with a recovery plan tailored to your needs.
The concept of the body “rejecting” a hip implant is often misunderstood. Unlike organ transplants, where the body can reject foreign tissue, hip implants are made from biocompatible materials such as titanium, cobalt-chromium alloys, and medical-grade polyethylene, which are designed to be accepted by the body.
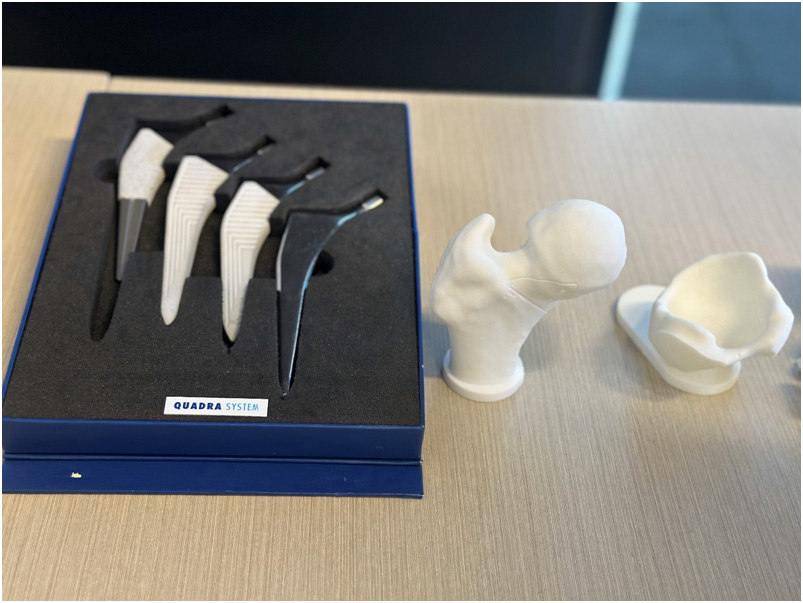
There are however a few related concerns that patients should be aware of:
Immune Response and Implant Tolerance: The materials used in hip implants are biocompatible, meaning they are generally well-tolerated by the body and are unlikely to trigger an immune response similar to organ rejection. This is why rejection, in the traditional sense, does not occur with hip implants.
Allergic Reactions: In rare cases, some patients may have an allergic reaction to the metals used in the implant, such as nickel or cobalt. This can cause symptoms like pain, swelling, or a rash around the implant site. If you have known metal allergies, this should be discussed with Dr Tulloch before surgery, as there are alternative materials that can be used.
Aseptic Loosening: Over time, some implants may loosen from the bone without an infection present, a condition known as aseptic loosening. This is not a rejection but a mechanical issue where the bond between the implant and the bone weakens. This can happen due to wear and tear, bone loss, or other factors.
Infection: While not a rejection, an infection can occur around the implant, which may require treatment with antibiotics or, in severe cases, additional surgery. Maintaining good hygiene and following post-operative care instructions can help reduce the risk of infection.
While most hip replacements provide lasting pain relief and significantly enhance mobility, understanding the potential for an immune response and taking steps to mitigate these risks can help ensure the long-term success of the implant.
The most commonly reported problem after hip replacement surgery is pain and discomfort, particularly in the early stages of recovery. While hip replacement surgery is generally successful in alleviating chronic pain and restoring mobility, it is normal for patients to experience some degree of pain, swelling, and stiffness as they heal.

Common Post-Surgical Issues
Early Post-Operative Pain: It is typical to experience pain immediately after surgery, which gradually decreases over time. This pain is usually managed with medication and physical therapy, but if the pain persists or worsens, it may need further evaluation.
Chronic Pain: In some cases, patients may develop chronic pain due to nerve irritation, muscle inflammation, or issues related to the implant. This is less common but can occur and may require additional treatment.
Joint Stiffness:Some patients report stiffness in the hip joint, especially if they are not able to follow a consistent rehabilitation and physiotherapy regimen. This stiffness can limit the range of motion and may require ongoing physical therapy to improve flexibility and function.
Leg Length Discrepancy:After hip replacement surgery, some patients may notice a difference in leg length. This can lead to discomfort and may require corrective measures such as shoe inserts or, in rare cases, further surgery.
Infection:Although rare, infections can occur around the surgical site or deep within the new hip joint. Infections may cause pain, redness, swelling, and fever, and they require prompt medical attention.
Implant Loosening or Dislocation:Over time, some patients may experience loosening of the hip implant or, in rare cases, dislocation of the hip joint. This can lead to pain and instability and may necessitate revision surgery.
Regular follow-up appointments with Dr Tulloch are crucial for identifying and addressing any post-operative issues early. Monitoring your progress and adhering to the recommended rehabilitation plan are key to achieving the best possible outcome.
The process of bone growing into your hip replacement, known as osseointegration, is crucial for the stability and long-term success of the implant. On average, it takes about 3 to 6 months for bone to fully integrate with the implant, though this can vary depending on several factors, including the type of implant used, your overall health, and how well you adhere to post-operative care instructions.
Many modern hip implants are designed as “press-fit,” meaning they rely on the bone to grow into the surface of the implant to secure it in place. These implants often have a porous surface or are coated with materials like hydroxyapatite, which encourage bone growth.
Bone Growth Timeline
Initial Healing (0-6 Weeks): In the first few week’s post-surgery, the body begins forming a soft callus around the implant. This initial phase is crucial for setting the foundation for further bone growth.
Early Bone Growth (6 Weeks – 3 Months): During this period, the bone begins to mature and integrate more closely with the implant. You may start to feel more stable, but it’s important to avoid high-impact activities that could disrupt the integration process.
Full Osseointegration (3-6 Months): By the 3-to-6-month mark, significant bone growth should have occurred, securely anchoring the implant to your natural bone. Your surgeon will monitor this process through follow-up appointments and imaging studies.
In conclusion, while it generally takes about 3 to 6 months for bone to fully grow into a hip replacement, individual factors can influence this timeline. By following Dr Tulloch’s advice and attending regular follow-ups, you can support the osseointegration process and contribute to the long-term success of your hip replacement.
The lifespan of a hip replacement is a common concern for patients considering or undergoing the procedure. Thanks to advancements in surgical techniques, implant design, and materials, modern hip replacements are more durable and longer lasting than ever before.
The longevity of a hip replacement, can vary depending on several key factors:
Implant Quality and Design: High-quality materials such as ceramic, metal, and highly cross-linked polyethylene have significantly improved the wear resistance and longevity of hip implants
Surgical Technique:The use of advanced surgical techniques, such as minimally invasive approaches and patient-specific implants, can enhance the precision of the procedure, potentially leading to better outcomes and longer-lasting implants.
Patient Activity Level:The amount and type of activity can affect how long a hip replacement lasts. High-impact activities may increase wear on the implant, while a balanced, moderate level of activity can promote its longevity.
Patient Weight:Higher body weight can exert more pressure on the hip replacement, potentially accelerating wear.
Age at Surgery:Younger patients tend to be more active and may require revision surgery in the future, as the implant may wear out over decades of use.

On average, current hip replacements are expected to last between 20 to 25 years. It’s important to note that with ongoing improvements in implant technology and surgical methods, many patients find their hip replacements function well beyond these estimates.
After a hip replacement, most patients experience significant improvements in pain relief and mobility, allowing them to return to many of their daily activities.

To protect the longevity of the implant and ensure optimal outcomes, there are some considerations and potential lifelong restrictions to keep in mind:
Avoid High-Impact Sports: Activities that involve running, jumping, or high-impact movements, such as basketball, soccer, or long-distance running, are generally discouraged. These activities can place excessive stress on the hip implant, leading to increased wear and potential early loosening.
Limit Heavy Lifting: Lifting heavy objects can also put significant strain on the hip joint. Patients are advised to be mindful of lifting techniques and avoid carrying heavy loads.
Avoid Extreme Hip Flexion: Movements that involve deep bending of the hip, such as squatting or sitting on very low chairs, can increase the risk of dislocation, particularly in the early stages of recovery. While the risk of dislocation decreases over time, patients should still be cautious with these movements.
Twisting Motions: Sudden twisting or pivoting on the operated leg can also place stress on the implant, potentially leading to complications. Gentle, controlled movements are recommended.
Avoid Contact Sports: Sports that involve physical contact, such as football or rugby, are generally not recommended. The risk of falling or experiencing a direct blow to the hip can be dangerous for the implant.
Maintain a Healthy Weight: Keeping your weight within a healthy range is crucial to reducing stress on the hip implant. Excess weight can accelerate wear and tear on the joint, potentially shortening the lifespan of the implant.
Safe Sleeping Positions: It’s often recommended to avoid sleeping on the operated side for an extended period. Using pillows between your legs can help maintain proper alignment and reduce the risk of dislocation during sleep.
Daily Activities: While most daily activities can be resumed, patients are encouraged to be mindful of their movements, especially when bending, twisting, or lifting. Proper body mechanics can help protect the hip joint and prolong the life of the implant.
While there are some lifelong considerations and potential restrictions after hip replacement surgery, most patients can enjoy a wide range of activities and an improved quality of life. By following Dr Tulloch’s advice on activity levels, lifestyle modifications, and attending regular follow-up appointments, you can maximize the benefits of your hip replacement and reduce the risk of complications.
A common question among patients considering or recovering from hip replacement surgery is whether their new hip will ever feel “normal.” The answer varies from person to person, but many patients report that their hip replacement eventually feels very natural, allowing them to return to a wide range of activities with minimal discomfort.

Factors Influencing How Normal a Hip Replacement Feels:
Initial Recovery Period: During the first few months after surgery, it is normal to experience some stiffness, discomfort, and a sense of unfamiliarity with the new joint. As the body heals and you regain strength and mobility, these sensations typically diminish.
Long-Term Adjustment: For most patients, the hip continues to feel more natural as time goes on. By the one-year mark, many report that the hip feels close to normal, with little to no awareness of the implant during everyday activities.
Advanced Implant Materials: Modern hip implants are designed to closely mimic the natural anatomy of the hip joint, allowing for smooth movement and reducing the sensation of having a foreign object in the body.
Precise Surgical Techniques: Techniques like the direct anterior approach, which minimises damage to muscles and tissues, can contribute to a quicker and more natural feeling recovery. Dr Tulloch’s expertise in these techniques plays a significant role in how normal the hip feels post-surgery.
Strength and Mobility Training: Consistent participation in excercies and following a tailored rehabilitation plan are crucial for regaining normal function. Strengthening the surrounding muscles and improving flexibility can make the hip feel more natural over time.
Realistic Expectations: It’s important for patients to have realistic expectations. While many patients eventually forget they have an implant, others may always feel some degree of difference compared to a natural hip. This is typically minor and doesn’t interfere with daily activities.
Mental Adaptation: Adapting mentally to the hip replacement is also part of the process. As you become more accustomed to the new joint, the sensation of having a hip replacement usually fades into the background.
For many patients, a hip replacement can indeed feel quite normal after full recovery, with most returning to their daily activities without significant discomfort or awareness of the implant. Individual experiences vary, and some patients may notice minor differences compared to a natural hip
There is no strict cut-off age for hip replacement surgery. The decision to undergo hip replacement is based more on a patient’s overall health, level of pain, and impact on quality of life rather than age alone. Both younger and older patients can benefit from hip replacement surgery if they meet certain criteria.

Younger Patients and Hip Replacement
Pain and Quality of Life: The primary considerations for younger individuals include the level of pain and the reduced quality of life due to hip issues.
Revision Surgery: Younger patients are more likely to need revision surgery in the future due to the longer life expectancy and the wear on the prosthetic over time.
Older Patients and Surgical Consideration
Overall, Health: For older patients, the feasibility of the procedure is often determined by evaluating overall health rather than age itself.
Comorbidities: Common comorbidities such as cardiovascular disease, diabetes, and other conditions are carefully assessed to gauge the risk of post-operative complications. The focus is on ensuring that the benefits of surgery—pain relief and enhanced mobility—outweigh the potential risks.
There is no absolute age limit for hip replacement surgery. Instead, the decision is based on a thorough evaluation of the patient’s overall health, lifestyle, and the degree to which hip pain affects their quality of life. By focusing on these factors, Dr Tulloch aims to provide the best outcomes for patients of all ages.
Yes, after hip replacement surgery, you will likely need some special equipment or aids to assist with your recovery and mobility. These aids are designed to help you move safely, reduce the risk of complications, and support your return to daily activities. The type and duration of equipment use will vary based on your individual recovery progress.

Key Equipment and Aids for Post-Surgery Recovery:
Walkers and Crutches: Immediately following surgery, using a walker or crutches helps you maintain balance and offload weight from the operated hip, facilitating early mobilisation with reduced risk of injury.
Canes: As your strength and confidence improve, transitioning to a cane for additional support might be advised until you’re comfortable and secure walking unaided.
Raised Toilet Seats: To make sitting down and standing up easier and to avoid excessive bending at the hip, a raised toilet seat can be very helpful in the bathroom.
Shower Chair or Bench: Showering safely while avoiding slips and falls is paramount. A shower chair or bench can provide stability and comfort while bathing.
Reaching Aids: To avoid bending and twisting at the hip, tools like grabbers or reaching aids are useful for picking up objects from the floor or high shelves.
Sock Aid and Long Handled Shoehorn: Dressing aids can assist you in putting on socks and shoes without bending over, maintaining hip precautions and independence in dressing.
Compression Shorts: Immediately following surgery, compression garments or shorts may also be recommended to support the healing process and minimize swelling.
The need for these aids typically decreases as your recovery progresses, with most patients gradually transitioning to walking unaided within a few weeks to a few months. The timeline can vary depending on individual factors, such as your overall health, the complexity of the surgery, and how well you follow your rehabilitation plan.
The timeline for returning to work after total hip replacement surgery varies depending on the type of work you do, your overall health, and how well your recovery progresses. On average, most patients can expect to return to work within 6 to 12 weeks after surgery, but this can vary based on individual circumstances:
YOUR TYPE OF JOB:
Sedentary or Office Work: If your job involves sitting at a desk and minimal physical activity, you may be able to return to work as early as 4 to 6 weeks after surgery. However, you should be mindful of your posture and take regular breaks to move around and stretch.
Light Physical Work: For jobs that involve light physical activity, such as standing, walking, or occasional lifting, a return to work might be possible around 6 to 8 weeks after surgery.
Physically Demanding Jobs: If your work is physically demanding, involving heavy lifting, climbing, or manual labour, it may take 10 to 12 weeks or longer before you are ready to return. In some cases, modifications to your work duties or a phased return might be necessary.

YOUR RECOVERY PROGRESS
Individual Healing: The speed of your recovery will depend on factors such as your age, overall health, adherence to post-operative care instructions, and how diligently you follow your rehabilitation program. Regular follow-up appointments with Dr Tulloch will help monitor your progress and determine when it’s safe to resume work.
Pain Management and Mobility: Being able to manage pain effectively and having sufficient mobility to perform your job duties are crucial considerations when determining your return to work timeline.
WORKPLACE MODIFICATIONS
Phased Return: Some patients benefit from a phased return to work, starting with reduced hours or modified duties before gradually resuming a full work schedule.
Ergonomic Adjustments: Depending on your job, you might need to make ergonomic adjustments to your workspace, such as using a chair with better support or adjusting the height of your desk to avoid strain on your hip.
The timeline for returning to work after total hip replacement surgery varies depending on the physical demands of your job and your individual recovery progress. Most patients return to work within 6 to 12 weeks, but this can vary. Dr Scott Tulloch will work with you to develop a tailored plan, ensuring that you return to work safely and at the right time for your recovery.
The timing for when you can safely resume driving after total hip replacement surgery varies, largely depending on factors such as the side of your surgery, your overall recovery progress, and the type of vehicle you drive.

Generally, patients may begin to consider driving around 4 to 6 weeks post-surgery, assuming they meet certain criteria:
Narcotic Pain Medications:Narcotic pain medications can impair your ability to make quick decisions and react, which are essential for safe driving.Ensure that you have stopped using these medications and can manage pain without them before considering driving.
Strength and Mobility:You should have regained sufficient strength and mobility in your leg to operate the pedals without discomfort. This means you need to be able to perform an emergency stop effectively without pain or hesitation.
Right Hip Surgery: If your surgery was on the right hip, you might need more time before driving, as it directly affects the leg used for accelerating and braking.
Left Hip Surgery: For those with left hip surgery, driving a manual car can be particularly challenging, as the left leg is used for operating the clutch. This may require an extended recovery period before safely resuming driving.
General Guidelines and Recommendations
Post-Surgery Timeline: Most patients are ready to resume driving around 4 to 6 weeks after surgery, provided they meet the above criteria.
Legal and Safety Considerations: There are no specific regulations or formal guidelines from licensing authorities regarding driving post-surgery in Australia, but it’s crucial to consider safety and personal readiness.
Practical Steps to Resume Driving
Test in a Safe Environment: Start by practicing in a safe, controlled environment like a parking lot to get accustomed to the feeling and ensure you can react appropriately.
Short Drives: Begin with short drives to build confidence and ensure comfort.
Ergonomics: Adjust your seat and steering wheel to ensure optimal comfort and control.
Monitor Pain and Fatigue: Be mindful of any pain or fatigue that might affect your ability to drive safely.
Feeling fatigued three months after hip replacement surgery can be concerning, but it’s not uncommon. This prolonged fatigue can result from several factors as your body continues to heal and adjust.

Possible Reasons for Prolonged Fatigue:
Ongoing Healing: Your body is still in the healing process, using significant energy to repair tissue, manage inflammation, and integrate the hip prosthesis. This energy demand can leave you feeling more tired than usual.
Blood Loss and Anaemia: Even with minimal blood loss during surgery, some patients may experience postoperative anaemia, which can lead to feelings of fatigue as your body works to replenish lost red blood cells.
Activity Level:Both insufficient physical activity and overexertion during recovery can contribute to fatigue. While regular movement is important for recovery, pushing yourself too hard can drain your energy.
Disrupted Sleep Patterns: Pain, discomfort, and adjusting to new sleeping positions after surgery can disrupt your sleep, making it difficult to get the restful sleep needed for recovery.
Emotional Stress:The emotional and psychological stress of undergoing surgery and adapting to a new lifestyle during recovery can also contribute to prolonged fatigue.
Medication Side Effects:Some medications prescribed for pain management and inflammation post-surgery may have side effects, including drowsiness or fatigue.
Nutrition:Adequate nutrition is crucial during recovery. A diet lacking in essential vitamins and minerals can contribute to ongoing fatigue.
MANAGING POST-SURGICAL FATIGUE
Dr Tulloch emphasises a comprehensive approach to managing fatigue during recovery:
Regular Follow-up: It’s important to report prolonged fatigue during follow-up visits so Dr Tulloch can assess potential medical causes, such as anaemia or medication side effects.
Balanced Rehabilitation: Engaging in a balanced, physiotherapist-guided rehabilitation program helps ensure that you remain active at a level that supports recovery without overexertion.
Nutritional Assessment: Consulting a nutritionist can help ensure your diet is optimized to meet your healing and energy needs.
Good Sleep Hygiene: Establishing a routine that promotes restful sleep can significantly improve your energy levels.
If fatigue persists despite these measures, Dr Tulloch may recommend further assessment to rule out any underlying conditions that could be contributing to your tiredness. Remember, every patient’s recovery journey is unique, and maintaining open communication with your healthcare team is key to managing post-surgical challenges.
Yes, MRI (Magnetic Resonance Imaging) technology has advanced significantly, making it generally safe for individuals with hip replacements. It’s crucial however, to consult with your healthcare provider and the MRI technician to ensure proper protocols are followed, considering the specific type of hip replacement you have, and any potential risks associated. With proper precautions and expertise, the benefits of diagnostic accuracy often outweigh the minimal risks involved.
While the risks are minimal, there can be concerns such as heating of the metal components, magnetic interference, or image artifacts that can affect the quality of the MRI scan. These are typically managed with advanced MRI technology and protocols.
While cold weather doesn’t directly affect the integrity of a hip replacement, some individuals may experience increased discomfort or stiffness in their joints during colder temperatures. This phenomenon is generally more related to changes in barometric pressure and muscle tension rather than the hip replacement itself.
UNDERSTANDING THE IMPACT OF COLD WEATHER
Discomfort and Stiffness:Changes in barometric pressure can cause tissues around the joint to expand and contract, potentially leading to discomfort.
Muscle Tension: Colder temperatures can cause muscles to tighten and become stiffer, which might contribute to the sensation of joint stiffness or discomfort.
Increased Sensitivity: Some patients report increased sensitivity to pain in colder weather. This is likely due to the body’s natural response to cold, which can heighten the perception of pain and discomfort in areas that have undergone surgery.
MANAGING DISCOMFORT IN COLD WEATHER
Regular Exercise: Engaging in regular, gentle exercise helps maintain joint flexibility and reduces stiffness. Activities such as walking, swimming, or stationary cycling can be beneficial.
Warm-Up: Ensure proper warm-up exercises before any physical activity to reduce muscle tension and prevent stiffness.
Dress Appropriately:Wearing warm clothing, including layers, can help maintain body warmth and reduce muscle stiffness.

While cold weather may not directly impact the hip replacement implant itself, it can contribute to increased discomfort or stiffness due to changes in barometric pressure and muscle tension. By maintaining an active lifestyle, dressing warmly, and following Dr Tullochs advice, patients can effectively manage any weather-related discomfort.
Yes, absolutely! A hip replacement is meticulously engineered to provide strength and durability comparable to your original hip joint. Modern advancements in materials and surgical techniques ensure that hip replacements offer exceptional stability and functionality. While nothing can fully replicate the intricacies of your natural hip, a well-performed hip replacement can provide remarkable strength and reliability, allowing you to regain mobility and lead an active lifestyle with confidence.

STRENGTH AND DURABILITY OF HIP REPLACEMENTS
Advanced Materials: Modern hip replacements are made from highly durable materials such as titanium, ceramic, and highly cross-linked polyethylene. These materials are designed to withstand the significant stresses and strains experienced by the hip joint.
Biocompatibility: These materials are also biocompatible, meaning they are well-tolerated by the body and minimise the risk of rejection or adverse reactions.
Surgical Techniques:The implants are precisely engineered to mimic the natural movement of the hip joint, providing excellent stability and range of motion.
Minimally Invasive Approaches: Advanced surgical techniques, including minimally invasive approaches, reduce muscle and tissue damage during surgery, promoting faster recovery and stronger outcomes
Longevity:Hip replacements are designed to last many years, with current implants often lasting 15 to 25 years or more. The longevity of the implant can be influenced by factors such as the patient’s activity level, weight, and adherence to post-operative care instructions.
Functionality: Most patients experience significant improvements in pain relief, mobility, and overall quality of life following hip replacement surgery.
While a hip replacement cannot fully replicate the complexities of a natural hip, it offers strength and functionality that allow patients to return to an active lifestyle with confidence. By following the guidance of Dr Tulloch, and maintaining a healthy lifestyle, you can maximize the benefits of your hip replacement and enjoy improved mobility for many years.
It’s not uncommon for patients to experience a sudden increase of approximately 4.5-6.8 kilograms on the bathroom scale immediately following hip replacement surgery. But fear not, as this weight gain is merely temporary and primarily due to fluid retention.

During surgery, your body undergoes stress, prompting it to shift a significant amount of fluid from your bloodstream into the interstitial space surrounding your cells. To counteract this fluid shift and maintain blood pressure, we administer generous amounts of IV fluids throughout the procedure. In fact, it’s typical for patients to receive up to 3 litres of saline on the day of surgery alone, equating to approximately 4.5 kilograms of liquid.
This fluid retention continues for several days post-surgery, often accompanied by increased thirst and fluid intake. In the initial phase, you may find yourself consuming more fluids than you’re expelling, contributing to the temporary weight gain. However, around days 3-5 after surgery, you’ll likely experience a significant increase in urine output as your body strives to restore its normal fluid balance.
It’s important to note that any pre-existing urinary issues may become more apparent during this period as your body works to regulate its fluid levels. Rest assured, once your fluid balance returns to normal, these issues typically resolve.
As for the weight of the hip replacement implants themselves, they’re relatively lightweight. Made primarily of titanium, with a ceramic head and polyethylene liner, the combined weight closely matches that of the bone removed during surgery—typically around 0.3 kilograms.
The National Joint Registry (NJR) is an essential resource that collects and monitors data on joint replacement surgeries across various regions, providing invaluable insights into the performance and outcomes of these procedures.

The National Joint Registry Purpose, Function, and Significance:
Data Collection:The NJR systematically collects data on joint replacement surgeries, including hip, knee, ankle, elbow, and shoulder replacements.It tracks the types of implants used, the surgical techniques employed, and patient demographics to build a comprehensive database.
Performance Monitoring: The registry monitors the performance of different implants and surgical techniques over time.It aims to identify trends, successes, and potential issues with specific implants or procedures to improve patient outcomes.
Quality Assurance:By tracking the long-term success rates of joint replacements, the NJR provides a benchmark for quality assurance in orthopaedic surgery.It helps healthcare providers maintain high standards and identify areas for improvement in surgical practice.
Patient Safety:The NJR enhances patient safety by providing data that helps in the early detection of poorly performing implants.It ensures that only the most effective and reliable implants are recommended and used.
Clinical Research:The registry serves as a valuable resource for clinical research, enabling studies on the effectiveness and longevity of different joint replacement techniques and materials.Researchers and clinicians use NJR data to develop new strategies and improve existing practices in joint replacement surgery.
Informed Decision-Making:Patients and healthcare providers can use NJR data to make informed decisions about joint replacement surgery.The registry’s insights help patients understand the potential outcomes and risks associated with different implants and procedures.
Improving Outcomes:The NJR plays a critical role in improving the outcomes of joint replacement surgeries by providing evidence-based data.It helps in refining surgical techniques and selecting the best implants, leading to better patient satisfaction and longevity of joint replacements.
Policy and Regulation:The data from the NJR informs policymakers and regulatory bodies, guiding decisions on the approval and regulation of new implants and technologies.It supports the development of standards and guidelines for joint replacement surgeries.
Confidentiality:Patient information in the NJR is kept confidential and is only accessible to authorised personnel who need the data for monitoring and research purposes.Data is anonymized for research purposes to protect patient identity.
Patients can request access to their own data recorded in the NJR to understand their surgical outcomes and any subsequent follow-ups and healthcare providers use the data to improve clinical practices and patient care strategies.
For more detailed information about the National Joint Registry, you can refer to the following sources:https://aoanjrr.sahmri.com/
Is Total Hip Replacement Right For You?
If you’re unsure whether total hip replacement is the right option, Dr Tulloch will assess your medical history, symptoms, and lifestyle. He will discuss non-surgical options and help you decide on the best path forward.
If surgery is recommended, you will have the opportunity to ask questions and receive information on how to prepare. Informed decision-making is a vital part of your care.
If you’re considering total hip replacement surgery or want more information, you can book a consultation with Dr Scott Tulloch. During your appointment, he will answer your questions and discuss the best treatment options for your individual needs.
LEARN ABOUT
- ANTERIOR MINIMALLY INVASIVE TOTAL HIP REPLACEMENT
- REVISION HIP REPLACEMENT SURGERY
- HIP REPLACEMENT SURGERY FAQS
